By Ed Pfueller, UOAA Communications and Outreach Manager
There is a stoma clinic so good that some people anticipate it every two years and travel from halfway across the country to go to it.
This free stoma clinic is staffed by volunteer Wound, Ostomy and Continence (WOC) nurses and medical professionals and is always included as part of UOAA’s National Conference. This summer the conference is back and a few ordinary rooms of the Hyatt Regency Grand Cypress Resort in Orlando, Florida will be transformed into a bustling stoma clinic from August 14 through 16. This free stoma clinic is stocked with a wide variety of supplies donated from manufacturers and other ostomy-related companies, large and small, for people to sample.
“The WOC nurses are helpful, informative, and full of suggestions and encouragement.”
UOAA Board Member Laura Kaiser, APRN, A-CNS-BC, WOCN is organizing the clinic and volunteer nurses this year. “My colleagues in ostomy care are very generous and giving individuals and are always willing to offer guidance and advice within their specialty. Many ostomy nurses have been lifelines to people through crises. A clinic often allows a nurse a different perspective on life! Ostomy nurses from past conferences say this is the best and most fulfilling conference that they have attended.” She says.

The conference attendees feel gratitude for the nurses. Gail Jasne attended the conference and stoma clinic in 2019 and said, “The WOC nurses are helpful, informative, and full of suggestions and encouragement.”
Mary Hardee attended the conference for the first time in 2023. “My first session was the free stoma clinic. The WOC nurse was very knowledgeable, reassuring and helpful. She let me try a different appliance that met my needs better and she gave me samples to try at home. She also noted that I have a hernia and educated me on that.” Hardee says.
Kaiser says stoma clinic patients should expect to be asked helpful questions to get the root of problems such as:
- Is your skin red and irritated, does the pouching system leak?
- Please describe what happens when the pouch leaks and where does it leak?
- What time do you eat your dinner?
- Show me how you clean your skin.
- Does your stoma or the skin around your stoma bleed?
- Patients often cut the wafer too large or too small and crust incorrectly, I always ask if I may measure their stoma.
- What pouching system lasted longest and was the most comfortable / what is the longest wear time?
UOAA believes that the best ostomy clinic is the one you can visit the soonest to solve an ostomy problem before it gets worse. That’s why we created the Ostomy Outpatient Services Locator to search for the one closest to you and champion the UOAA Virtual Ostomy Clinic with The Wound Company for a self-pay solution you can access wherever you are.
Jill Jeffries shared her experience and perspective meeting other ostomates gave her. “The nurse explained how I could better wear my pouch system to protect my stoma and surrounding skin from possible irritation. Many people I met had much more serious issues than mine, and I left with a few new friends and great gratitude that my situation is so manageable. I also took away several samples of products new to me that I believe will be very helpful,” Jeffries said. “Thank you for such a great opportunity! I hope to see everyone at the next UOAA National Conference.” she added.
“She let me try a different appliance that met my needs better and she gave me samples to try at home.”
As for the ostomy supply samples that will be available this summer Ostomy Nurse Kaiser says, “If all of the manufacturers come through then the inventory should be extensive and will offer patients and nurses alike a great opportunity to see what is available to the consumer.”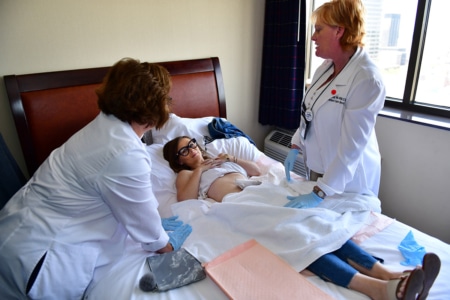
There are typically 18 to 30 volunteers helping in the stoma clinic so Kaiser says if they have enough nurses this year, one WOC Nurse will see patients and make recommendations and be paired with another medical professional (who may or may not be an ostomy nurse) who would act as a runner, assistant and overall helper.
“The stoma clinic along with our huge ostomy product exhibit hall is something that really makes UOAA National Conferences so unique,” says UOAA President Cheryl Ory. “There are people who very infrequently see an ostomy nurse but when they arrive at our conference always check in at our stoma clinic to see what small improvements they may be able to make in their ostomy health.”
This year the free stoma clinic will be open 8:00 am to 5:00 pm Thursday, August 14 and Friday August 15 and 8:00 am to Noon on Saturday, August 16.
“Conference registrants can sign-up through our new conference mobile app by selecting the time slot that works for them and add it to their calendar of sessions and events, or in-person at the information desk when they arrive to check in,” says UOAA Executive Director Christine Ryan.
Thank you to the the companies that donate supplies and the nurse volunteers who provide this service to our community at each UOAA National Conference!



 40 vendors will be there to visit with you and share any new products they are offering, services they provide, clothing and accessories available in today’s market, and much more. We’ll be serving a complimentary boxed lunch on Friday before the Exhibit Hall closes at 1pm for you to enjoy.
40 vendors will be there to visit with you and share any new products they are offering, services they provide, clothing and accessories available in today’s market, and much more. We’ll be serving a complimentary boxed lunch on Friday before the Exhibit Hall closes at 1pm for you to enjoy.
 UOAA’s 9th National Conference. Stay a few days earlier or after the conference and enjoy what the Resort has to offer with family and/or friends.
UOAA’s 9th National Conference. Stay a few days earlier or after the conference and enjoy what the Resort has to offer with family and/or friends.

 signing onto ten different letters that were sent to Congress many with positive results and we had several open action alerts on our advocacy platform supporting Federal legislation. We also continue to advocate with the Access and Care Coalition in our efforts with the Medical Directors from the Centers of Medicare and Medicaid Services (CMS) to make improvements to the ostomy policies and processes in particular for those beneficiaries who medically need greater quantities of products than what is allowable under the current policy. We won’t stop until this is resolved. Another example has been challenges with
signing onto ten different letters that were sent to Congress many with positive results and we had several open action alerts on our advocacy platform supporting Federal legislation. We also continue to advocate with the Access and Care Coalition in our efforts with the Medical Directors from the Centers of Medicare and Medicaid Services (CMS) to make improvements to the ostomy policies and processes in particular for those beneficiaries who medically need greater quantities of products than what is allowable under the current policy. We won’t stop until this is resolved. Another example has been challenges with 



