Have you ever wondered what you should be doing to fill your time as you recover from ostomy surgery?
After my first surgery at the age of 17, and even after my third surgery at the age of 23, I spent most of my time lounging around my parents’ house, waiting for the day that I would be cleared by my surgeon to return to “normal” activity. My parents would coax me out of the house to go on one walk a day, but I spent almost all of my time watching television and YouTube videos and sleeping.
Fast forward to age 30. At age 30, I ended up having my sixth major abdominal surgery. And by this point in time, I had been working as an Occupational Therapist (OT) in a hospital setting for six years. For six years, I had been helping other individuals recover and rehabilitate from major illness and injury. I had also spent years recreating in the mountains and enjoying a highly active lifestyle. So when I found out that I needed a stoma revision, I knew that my recovery would look very different from my previous surgeries. I knew that in order to improve my recovery time, decrease my risk for complications, and get back to the mountains, I had to put in more work.
enjoying a highly active lifestyle. So when I found out that I needed a stoma revision, I knew that my recovery would look very different from my previous surgeries. I knew that in order to improve my recovery time, decrease my risk for complications, and get back to the mountains, I had to put in more work.
For those who are less familiar with the rehabilitation professions, “Occupational Therapists enable people of all ages to live life to its fullest by helping them promote health, and prevent – or live better with – injury, illness, or disability” [1] and “Physical therapists [PTs] are movement experts who improve quality of life through prescribed exercise, hands-on care, and patient education” [2]. Although I’m an OT, seeking out my own rehab professional to work with was the best thing I could have done.
I already knew a lot of the basics of how to rehab myself, but having someone else who I would be accountable to and who I could bounce ideas off of was a bonus. I knew from my training as an OT that one 30-min therapy session prior to abdominal surgery, reduces the risk of complications by 50% [3]. So the first thing I did was set up an appointment with a pelvic health therapist prior to my surgery. I was able to find a local pelvic health PT to work with, although, both OTs and PTs may specialize in pelvic health. I sought out a pelvic health therapist because of her specialty training in digestive and urinary systems and the interaction between the abdomen and pelvic floor. In my time working as an OT, and in my time spent working with many PTs, I’ve learned that there are fundamental areas that ostomates should be targeting after surgery to improve their outcomes. Working with a therapist in the following areas can be quite beneficial:
Therapeutic Breathwork. Breath is necessary for life. If you aren’t breathing properly, you certainly won’t be getting back up on your feet and recovering from surgery any time soon. Breathing properly can also help decrease the pressure in your abdomen (i.e. intra-abdominal pressure) which decreases your risk for parastomal hernia and other complications.
Mobility Training. Focusing on walking in a strategic manner following surgery can also set you up for success in the long run. Not only is walking good for building up your endurance again, but it is a great way to begin engaging your core in a gentle manner.
Core Recovery. After surgery, your abdomen can be very tender. But it’s important to begin exercising in order to coordinate your abdominal muscles again and gain strength so that you will be less likely to injure yourself in the future.
Functional Daily Activities. Finally, as you go about your day-to-day routine, some tasks will feel more difficult than they used to. For example, bending to put on your socks can be painful and can pull at your incision. Working with a therapist on strategies to increase your independence and return to the daily activities you enjoy is invaluable.
I’m lucky that I decided to become an Occupational Therapist. It has enabled me to empower myself with knowledge about the human body and recovery from surgery. But you don’t have to be a therapist to have a positive recovery experience and lead a fulfilling life. If you’re feeling stuck, seek out a rehabilitation professional. You deserve quality care and support to feel confident and strong after surgery.
Wishing you well on your ostomy journey,
Charlotte
 As you start your journey to recovery, you’ll experience that life after ostomy surgery is a new reality. No matter how far after surgery you are, you will need to adapt to your condition and cope with your new situation. If you’re looking for additional support during your ostomy journey, consider enrolling in Coloplast’s free online support program, Coloplast® Care! It is a personal product support program designed in collaboration with nurses to provide you with individualized product support and lifestyle education, and product access coordination. Coloplast Care is available when you need it – whether it is through our online educational resources offering reliable product and lifestyle advice, news and tips customized for your situation, or over the phone with our team of dedicated Ostomy Advisors. We’re here to help!
As you start your journey to recovery, you’ll experience that life after ostomy surgery is a new reality. No matter how far after surgery you are, you will need to adapt to your condition and cope with your new situation. If you’re looking for additional support during your ostomy journey, consider enrolling in Coloplast’s free online support program, Coloplast® Care! It is a personal product support program designed in collaboration with nurses to provide you with individualized product support and lifestyle education, and product access coordination. Coloplast Care is available when you need it – whether it is through our online educational resources offering reliable product and lifestyle advice, news and tips customized for your situation, or over the phone with our team of dedicated Ostomy Advisors. We’re here to help!
Visit us at www.ostomy.coloplastcare.us or call 1-877-858-2656.
Information from Coloplast® Care is for educational purposes only. It is not intended to substitute for professional medical advice and should not be interpreted to contain treatment recommendations.
About the author:
Charlotte Foley, MS OTR/L, CBIS, received her Occupational Therapy degree at Boston University and began her career in the adult Inpatient Rehabilitation setting. She now works in the adult Acute Care setting at Providence Alaska Medical Center in Anchorage, Alaska. Because of her own personal and professional experience, Charlotte founded and runs her own education and consulting business, Restorative Ostomy Solutions, to empower individuals to feel strong and confident as they recover from ostomy surgery.
Charlotte has received compensation from Coloplast to provide this information.
Editor’s note: This article is from one of our digital sponsors, Coloplast. Sponsor support along with donations from readers like you help to maintain our website and the free trusted resources of UOAA, a 501(c)(3) nonprofit organization.
References
[1] AOTA (2021). What is Occupational Therapy? Retrieved from
https://www.aota.org/conference-events/otmonth/what-is-ot.aspx.
[2] APTA (2021). What Physical Therapists do? Retrieved from
https://www.apta.org/your-career/careers-in-physical-therapy/becoming-a-pt.
[3] Boden, I., Skinner, E., Browning, L., Reeve, J., Anderson, L., Hill, C., Robertson, I., Story,
D., & Denehy, L. (2018). Preoperative physiotherapy for the prevention of respiratory complications after upper abdominal surgery: pragmatic, double blinded, multicentre randomised controlled trial. British Medical Journal, 360:j5916. http://dx.doi.org/10.1136/bmj.j5916

 The seatbelt wrapped around my waist and caused me to lose blood flow to my intestines, which then had to be removed. I was left with no absorptive function and diagnosed with SBS. Though some people may arrive at an SBS diagnosis as a result of other gastrointestinal (GI) conditions, my introduction to SBS was abrupt. One day I was a college basketball player and homecoming king. The next I woke up in the ICU being told I would likely never eat or drink again.
The seatbelt wrapped around my waist and caused me to lose blood flow to my intestines, which then had to be removed. I was left with no absorptive function and diagnosed with SBS. Though some people may arrive at an SBS diagnosis as a result of other gastrointestinal (GI) conditions, my introduction to SBS was abrupt. One day I was a college basketball player and homecoming king. The next I woke up in the ICU being told I would likely never eat or drink again.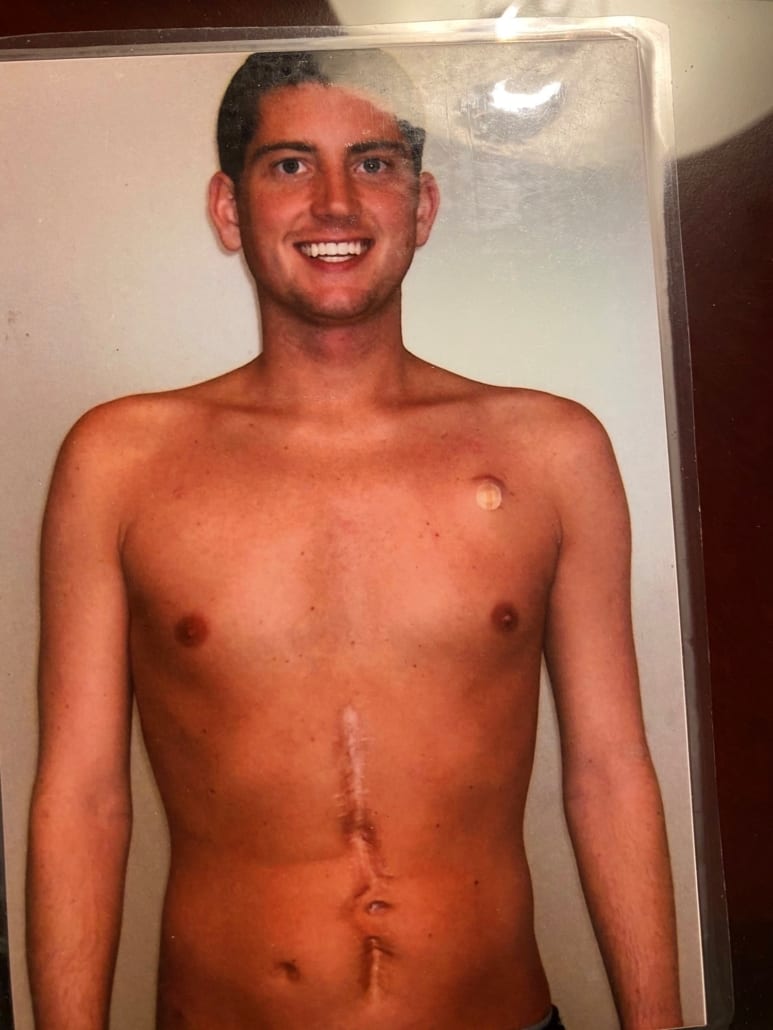 journey! But despite triumphing over those physical challenges, I had more hurdles to face, particularly in terms of my mental and emotional health.
journey! But despite triumphing over those physical challenges, I had more hurdles to face, particularly in terms of my mental and emotional health.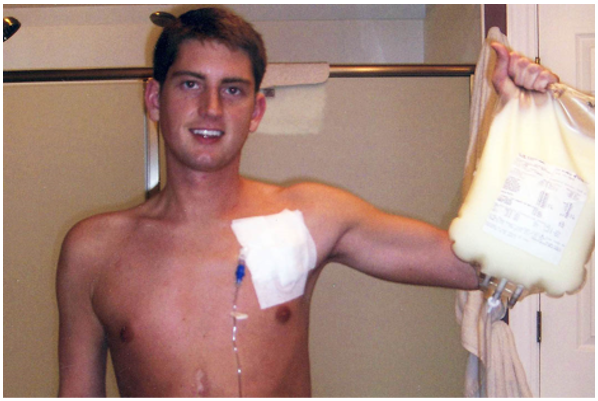


 publication of the UOAA), which still exists today. Not long after, I got America Online (AOL) and felt like I was on the forefront of technology. I had a computer, and now the internet. Imagine horns blasting – my world opened up and the exchange of information worldwide was awesome. Even more ways to communicate! A woman in Colorado who read my book, “If the Battle is Over, Why am I Still In Uniform,” emailed me, decided to get a colonoscopy, and was spared from cancer. That is a satisfying feeling, to know you gave up a year of your life to write a book and it saved another.
publication of the UOAA), which still exists today. Not long after, I got America Online (AOL) and felt like I was on the forefront of technology. I had a computer, and now the internet. Imagine horns blasting – my world opened up and the exchange of information worldwide was awesome. Even more ways to communicate! A woman in Colorado who read my book, “If the Battle is Over, Why am I Still In Uniform,” emailed me, decided to get a colonoscopy, and was spared from cancer. That is a satisfying feeling, to know you gave up a year of your life to write a book and it saved another.


 nurses) would recommend 3‐5 days of wear time. What I would definitely advise against is waiting until you HAVE to change due to a leak. Before you realize you have a problem, waste is coming into contact with your peristomal skin, and that may lead to skin damage. Above all, you want to keep your skin healthy, happy and intact. So when would my daily activity impact my wear time? Again it’s moisture math! I mentioned earlier that I like to swim and jacuzzi; a quick dip for an hour or so is very different than a big day out that involves being in a wet bathing suit all day. If I am planning a big day out on the water, in the pool, at a beach or waterpark, I figure that in to my changing schedule. For example if day one was Thursday, and day three is a big day out involving water, when I get home, I’ll typically shower and do a full change.
nurses) would recommend 3‐5 days of wear time. What I would definitely advise against is waiting until you HAVE to change due to a leak. Before you realize you have a problem, waste is coming into contact with your peristomal skin, and that may lead to skin damage. Above all, you want to keep your skin healthy, happy and intact. So when would my daily activity impact my wear time? Again it’s moisture math! I mentioned earlier that I like to swim and jacuzzi; a quick dip for an hour or so is very different than a big day out that involves being in a wet bathing suit all day. If I am planning a big day out on the water, in the pool, at a beach or waterpark, I figure that in to my changing schedule. For example if day one was Thursday, and day three is a big day out involving water, when I get home, I’ll typically shower and do a full change.



