By Robin Glover
Oh, the holidays! When cookies, cakes, and delicious pies suddenly appear everywhere, beckoning you to indulge in their sugary goodness. Don’t forget about those casseroles and their incredible aromas billowing from underneath a melted cheese topping. And those nuts — salty little kernels of flavor often found hiding among the decadently seasoned pretzels and cereal in everyone’s favorite snack mix.
The holidays are delicious, and food and drink are some of the many traditions friends and families have shared for generations. But, for people with an ostomy, eating and drinking around the holidays isn’t just a matter of likes and dislikes. Depending on the individual, certain things should be avoided while others can be enjoyed with no issues. The following is a guide to holiday eating (and drinking) with an ostomy.
It’s important to remember that these are general guidelines. Everyone is different, and each person experiences food differently. Consult with your physician or a registered dietician to know what’s best for you.
That being said, there’s no reason your ostomy, whether a colostomy, ileostomy, or urostomy, should hold you back from enjoying many, if not most, of your favorite holiday treats.
Maintain a Balanced Diet
Even during the holidays, maintaining a balanced diet is vital. No matter how good those sweets look, keep in mind that excess sugar and high-fat content can cause diarrhea, leading to the malabsorption of nutrients, leaving you feeling tired, irritable, and not in the holiday spirit. That doesn’t mean you need to deprive yourself, though. Just choose wisely.
not in the holiday spirit. That doesn’t mean you need to deprive yourself, though. Just choose wisely.
For those with a urostomy, choosing non-citrus foods high in Vitamin C can lower the risk of infections. Examples of these include cranberries, broccoli, potatoes, strawberries, and leafy vegetables.
Chew Your Food Thoroughly
And while you’re at it, chews wisely too. For those with an ileostomy or short bowel, this is especially important. Both of these reduce the time your body has to digest the food you eat. Chewing your food a little extra can go a long way in helping your body get the nutrients it needs.
Eat Small Meals
Don’t forget to take breaks throughout the day to have a small meal or nutritious snack, even while you’re busy wrapping presents, decorating, and socializing. Eating several small meals is more beneficial than waiting to eat one large meal at the end of the day. An empty stomach can also be a source of gas.
Focus On Hydration
With all the hustle and bustle of the holidays, it’s easy to forget about the need to stay hydrated. That’s why it’s even more important to focus on good hydration during the holiday season. This includes drinking plenty of water while trying to limit drinks with added sugars, artificial colors or sweeteners, caffeine, or alcohol. Aim for 8-10 glasses of water a day.
Water alone won’t do it, though. Your body needs electrolytes, too. Sports drinks are a good source for this. However, you should dilute them with water to lower the sugar concentration. Electrolyte drops are also a good solution.
Low electrolyte levels can lead to many undesirable effects, including fatigue, irritability, and nausea. These symptoms only get worse the more dehydrated you get. So drink up!
If you have a urostomy, it’s crucial to drink plenty of water to avoid possible urinary tract infections (UTIs). And, since it’s recommended to consume plenty of Vitamin C, enjoy some holiday apple cider too!
Depending on the individual, certain things should be avoided while others can be enjoyed with no issues.
Ask About Ingredients
Things like casseroles, dips, cultural specialties, and cakes can often include ingredients you might not notice right away. During the holiday season, nuts can often be the biggest culprits and can cause discomfort or even a dangerous blockage for those with an ileostomy and to a lesser extend a colostomy. Other foods to be careful of are corn, if not fully ground in dishes like tamales, and dried fruits. Skip over foods, as tempting as they may be, that may include any of your trigger foods. Don’t worry; it’s ok to ask. Many people avoid certain foods for all kinds of reasons.
Know Your Safe Foods
If you want to play it safe this holiday season, then stick to foods you know your body handles well. Consider keeping a food journal to help you keep track for next year. If you’ve recently had surgery for a colostomy or ileostomy, keep in mind these foods to avoid, but know that through trial and error you should soon feel more confident you’ll be able to enjoy most all of your holiday favorites.
Please read UOAA’s Eating With An Ostomy guide for more comprehensive information.
Robin Glover is a writer based in the Houston area. He has a permanent ostomy after being diagnosed with Crohn’s Disease in 2017.


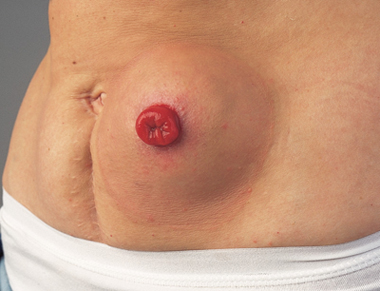 intestine and the weak spot is in the same area the surgeon created your stoma.
intestine and the weak spot is in the same area the surgeon created your stoma.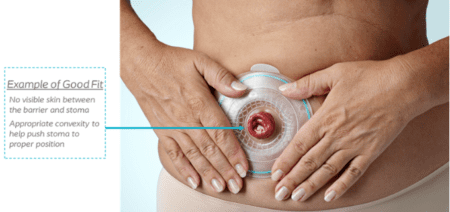
 Mackenzie Bauhs, CWOCN, is currently an employee and Ostomy Clinical Consultant for Coloplast. She obtained her bachelor’s degree at Carroll University in Wisconsin. She has worked with ostomy patients in the post-operative period at the University of Wisconsin Hospital and Clinics in Madison, Wisconsin as well as outpatient ostomy care at Rush University Medical Center in Chicago, Illinois.
Mackenzie Bauhs, CWOCN, is currently an employee and Ostomy Clinical Consultant for Coloplast. She obtained her bachelor’s degree at Carroll University in Wisconsin. She has worked with ostomy patients in the post-operative period at the University of Wisconsin Hospital and Clinics in Madison, Wisconsin as well as outpatient ostomy care at Rush University Medical Center in Chicago, Illinois.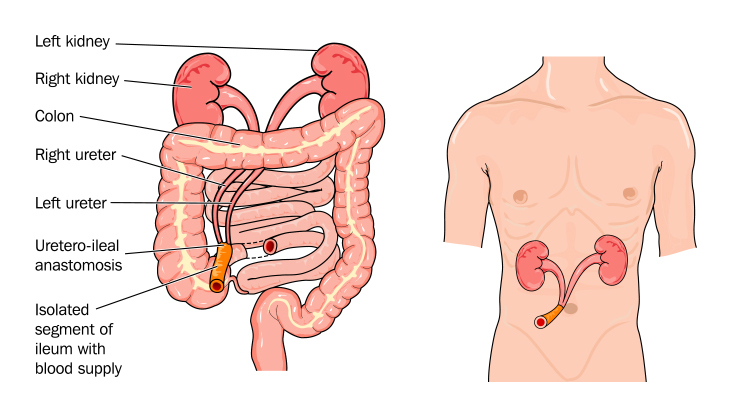 Why Do People Need A Urostomy?
Why Do People Need A Urostomy?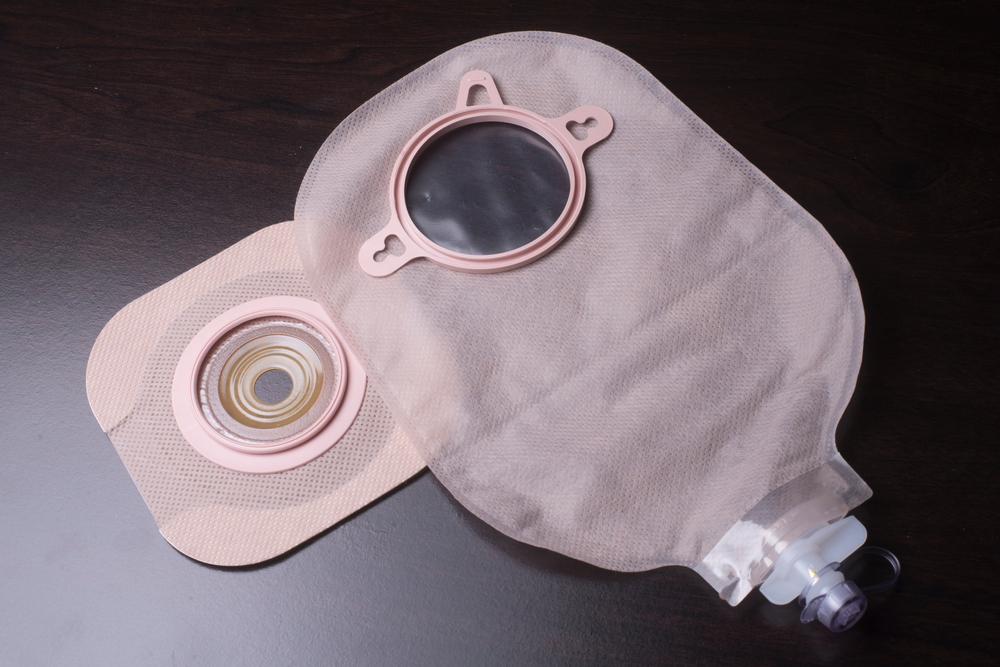
 not in the holiday spirit. That doesn’t mean you need to deprive yourself, though. Just choose wisely.
not in the holiday spirit. That doesn’t mean you need to deprive yourself, though. Just choose wisely. As a person with a complicated medical history, I was definitely paying attention, and started taking precautions very early to mitigate risk. As anyone who lives with a compromised immune system and chronic illness knows, when we get sick, it can have a way of snowballing.
As a person with a complicated medical history, I was definitely paying attention, and started taking precautions very early to mitigate risk. As anyone who lives with a compromised immune system and chronic illness knows, when we get sick, it can have a way of snowballing.


