Caring for a child with short bowel syndrome (SBS), a serious and chronic malabsorption disorder, can often feel isolating and disheartening.1, 2, 3 Unexpected barriers and challenges can make the condition difficult to manage and live with. And, because SBS is rare, finding information and support can be especially difficult. But for my daughter Mariah and me, this life with SBS is not about injustice, it’s about empowerment – a lesson Mariah has taught me better than anyone. As she puts it, “Mommy, I picked this life, and I picked you to be here to do it with me.”
Hearing those words years ago through the smile of my young daughter has been the ultimate source of strength for me. Mariah was born with most of her small bowel and half of her colon missing and was diagnosed with SBS at birth. She doesn’t receive nutrients as well as she should, which can lead to malnutrition, dehydration and other physiological complications. However, she was also born with incredible, innate resilience – that resilience has empowered me to break down walls and advocate fiercely on her behalf along our journey.
Finding strength has not always been easy. At the time of Mariah’s birth, the doctors said she would not live past one year. Essentially, I was told that my daughter had a death sentence. I did not accept that. But even though I didn’t doubt that she would survive her SBS diagnosis, I still grieved. Then, eventually I said to myself, “We will be the exception. We will be unique, and my child will thrive.” And, ultimately it was Mariah who created her own reality by not only surviving, but thriving. She simply shocked everyone.
Mariah is now ten years old, and she’s just like other kids in so many ways. For example, she certainly doesn’t like to clean her room! She is also her own wonderfully special person – she is a trickster who loves playing jokes on her brother and sister, and even kids around with nurses and staff during difficult hospital visits. She is equally nurturing and an avid caretaker of the sunflowers in our garden.
As Mariah gets older, I want to encourage her to become independent in every aspect of her life and to be curious about her SBS management. She already likes to gather her own supplies and has taken a particular interest in flushing out her own line (of her total parenteral nutrition [TPN]). Mariah doesn’t have the eating aversion that some kids with SBS might develop, so I allow her to eat whatever she wants and stock up her assigned “snack pantry” with what she chooses. Giving her the option to choose her own snacks is just one way that we’re building and supporting Mariah’s self-reliance in her SBS care and daily life.
This sense of independence helps Mariah feel like her true self because, as other parents of children with SBS likely know, the disease is not always pretty. That was especially true of Mariah’s experience following a surgical procedure known as an ileostomy. An ileostomy is a surgically created opening from the ileum, the lowest part of the small intestine. The intestine is brought through the abdominal wall to form a stoma. We agreed to do the ileostomy after she had been experiencing incredible pain when trying to use the bathroom. She would have acidic bowel moments and fissures – it was just awful.
The ileostomy was a temporary solution at best but was by no means perfect. We never had enough bags (or ileostomy pouches) and living with an ileostomy was challenging for us. At Mariah’s school, I would try to encourage curiosity and acceptance by telling the other kids that Mariah was an “alien from another planet” to explain her pouch. While a somewhat satisfactory explanation for most of the kids, she still experienced bullying from some of them. Thankfully, Mariah has always been confident in letting those bullies know that even if they weren’t being very nice, she would love them anyways. She punished them with kindness. It’s just another one of those things that makes her “Mariah”. Ultimately, Mariah was able to have the ileostomy reversed a few months ago which was a relief to us all.
In the moments of struggle that come with her SBS, Mariah has always responded with even greater moments of strength – sometimes even more strength than I possess myself. She has already had 40 surgeries in her first ten years of life, and on one occasion I decided to do her makeup with “winged” eyeliner before her procedure. However, when she came out of surgery, her makeup had been smeared. When she saw that I was crying, I told her the white lie that it was over the ruined eyeliner rather than let her see how hard it was watch her endure another challenge. Yet she was the one who said, with an unbothered smile, “Mom, stop! It’s not that serious, we’ll fix it later.” Her spirit is my strength, and that spirit inspires me to advocate fiercely for her every day.
In general, I feel there needs to be greater advocacy for the lives touched by SBS. It’s rare, and in my experience, there aren’t many people who can bridge the gap between parents’ understanding of the condition and the knowledge that medical professionals have. Although people living with SBS often have a circle of care that includes healthcare professionals across various disciplines, it can be difficult to merge everyone’s insights and get on the same page.
I have learned that to speak the same language as medical professionals, you must be invested and passionate about your research. For me, Google is my best friend. I research online to understand things like the vascular system and other biological processes. I read medical case studies online. I look at clinical studies. I constantly do my own fact-finding because I want to understand how a treatment will impact my child. The best way to do that is by arming myself with information as I fight to ensure she receives the care and treatment plans that are most appropriate for her.
It can take time to find medical professionals who are comfortable when a parent says, “I respect your opinion, but I’ve done my research, as well, and we’re not going to do that; we’re going to do this instead.” I’ve learned that you can, in fact, get through brick walls. Although sometimes it’s by going over, around or under versus breaking through. And when medical professionals don’t think I’m at their level, I have no problem “putting on my heels” to get there so they hear me.
Although I am not a physician, I do have a PhD in Mariah – no one knows her better than I do. I know that when she has an infection, her eyes will turn bright green. When she’s going to have a fever, she sleep talks. I’m compelled to ask the deeper questions about why a doctor may believe a new treatment or procedure is necessary. This sometimes has forced us to switch providers because in my view, “protocols” are not personalized to Mariah’s needs. Every person with SBS has a unique experience.
We are ALL human, doctors included. And we can make mistakes, learn and grow. All the things that I didn’t know when Mariah was diagnosed with SBS have helped me remain teachable and earnest in advocating for her. I’ve learned so much more by recognizing what I don’t know. Being humble enough to take advice has given me the greatest defense.
Nevertheless, it is challenging to constantly find resources and support, especially as a single parent. Trying to make ends meet at home while managing Mariah’s SBS journey is an ongoing challenge. Even when reaching out to other parents in the SBS community, it can be difficult to find balance. But the biggest support I find is that I don’t feel alone. When I talk to other parents in the community about our experiences, they just get it. I don’t have to explain Mariah’s condition or worry I will feel crazy. I can just ask, “Do you experience this?” and they say, “Yes, we got you!” Immediately, I feel less alone.
This journey takes strength and resilience, there is no doubt about it. Even with the support of the community and loved ones, ultimately, no one really knows what it takes for Mariah to be Mariah. They don’t know she has to carry a backpack for her nutrition. They don’t know what it looks like when I have to hold her for 15 minutes after her three daily shots. But they do see her strength, and they are compassionate towards the way Mariah knocks down every obstacle in her way, even those that would probably defeat others. I am humbled that this is our walk, and I believe it was given to us for a reason.
Just as the community encourages me and reminds me that I am not alone, I hope to encourage others in the community who may just be starting out on their SBS journey or struggling along the way. When talking to parents of newly diagnosed children, I want them to know that every child is unique, like a fingerprint. It’s all about believing that your child can do what they need to do. The most important thing is to know you’re doing the best for your child at every step of the way. This condition does not have to be a death sentence. And, if your child is anything like mine, he or she is likely stronger than you ever could have imagined.
To learn more about Short Bowel Syndrome (SBS), visit https://www.shortbowelsyndrome.com/. To join the community and talk with others who are living with SBS, check out https://www.facebook.com/TakedaSBS.
This article was created by Takeda.
Editor’s Note: This educational article is from one of our digital sponsors, Takeda. Sponsor support along with donations from our readers like you help to maintain our website and the free trusted resources of UOAA, a 501(c)(3) nonprofit organization.

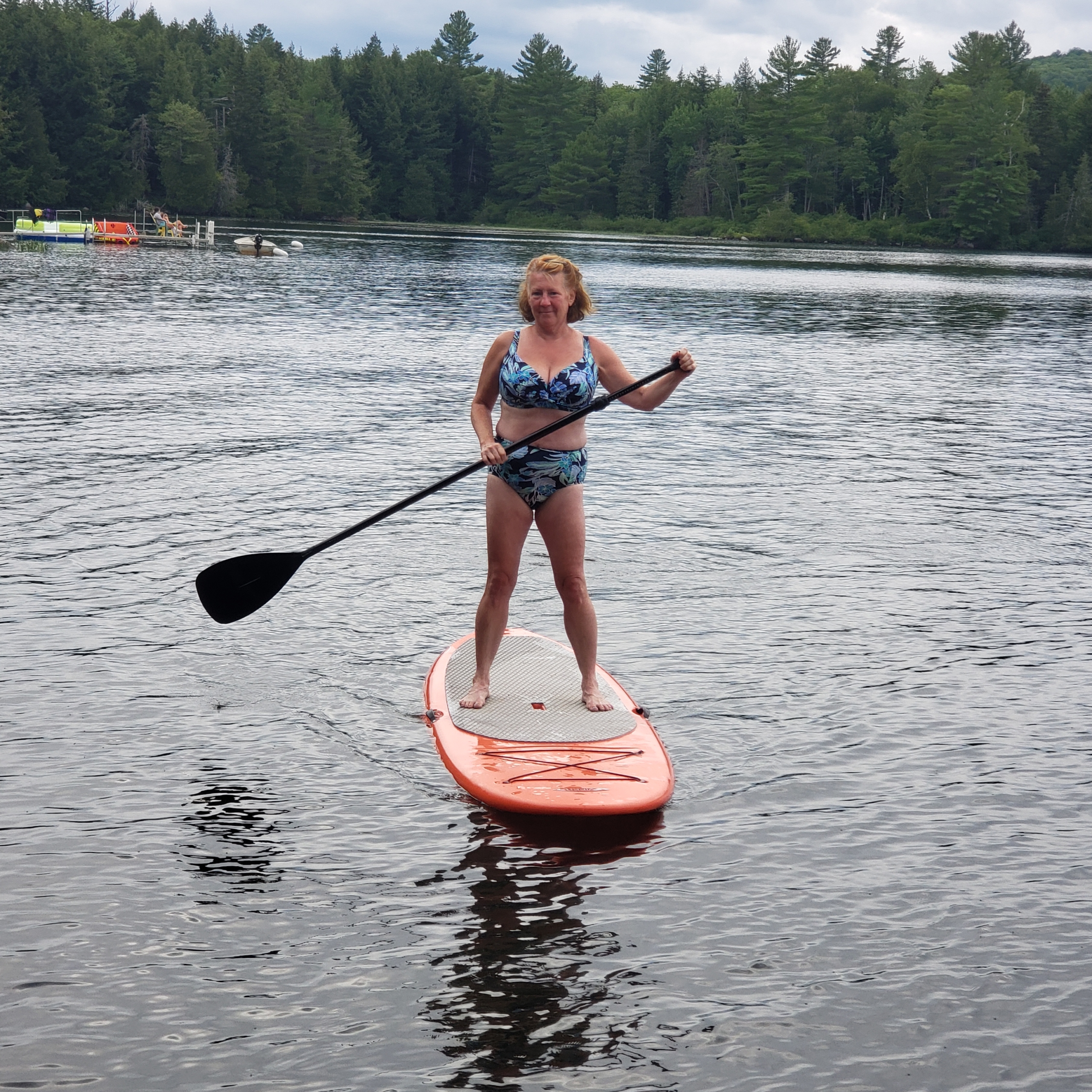 So, what can I do now that I have a urostomy?
So, what can I do now that I have a urostomy? There are so many other things I have been able to do since my
There are so many other things I have been able to do since my 
 I’m thankful for all of the WOCNs I have been to. Some I’ve known for many years. They are very knowledgeable and helpful with various products.I also want to give a shoutout to our great WOCNs at 11 Health & Technologies for being amazing for our team and patients. ? –Megan Alloway
I’m thankful for all of the WOCNs I have been to. Some I’ve known for many years. They are very knowledgeable and helpful with various products.I also want to give a shoutout to our great WOCNs at 11 Health & Technologies for being amazing for our team and patients. ? –Megan Alloway I want to tell my story concerning my ileostomy in order for people to understand how it is living with one and how a person can live a normal life and more.
I want to tell my story concerning my ileostomy in order for people to understand how it is living with one and how a person can live a normal life and more.



 nurses) would recommend 3‐5 days of wear time. What I would definitely advise against is waiting until you HAVE to change due to a leak. Before you realize you have a problem, waste is coming into contact with your peristomal skin, and that may lead to skin damage. Above all, you want to keep your skin healthy, happy and intact. So when would my daily activity impact my wear time? Again it’s moisture math! I mentioned earlier that I like to swim and jacuzzi; a quick dip for an hour or so is very different than a big day out that involves being in a wet bathing suit all day. If I am planning a big day out on the water, in the pool, at a beach or waterpark, I figure that in to my changing schedule. For example if day one was Thursday, and day three is a big day out involving water, when I get home, I’ll typically shower and do a full change.
nurses) would recommend 3‐5 days of wear time. What I would definitely advise against is waiting until you HAVE to change due to a leak. Before you realize you have a problem, waste is coming into contact with your peristomal skin, and that may lead to skin damage. Above all, you want to keep your skin healthy, happy and intact. So when would my daily activity impact my wear time? Again it’s moisture math! I mentioned earlier that I like to swim and jacuzzi; a quick dip for an hour or so is very different than a big day out that involves being in a wet bathing suit all day. If I am planning a big day out on the water, in the pool, at a beach or waterpark, I figure that in to my changing schedule. For example if day one was Thursday, and day three is a big day out involving water, when I get home, I’ll typically shower and do a full change.
